Who Will Lose Health Insurance With New Bill
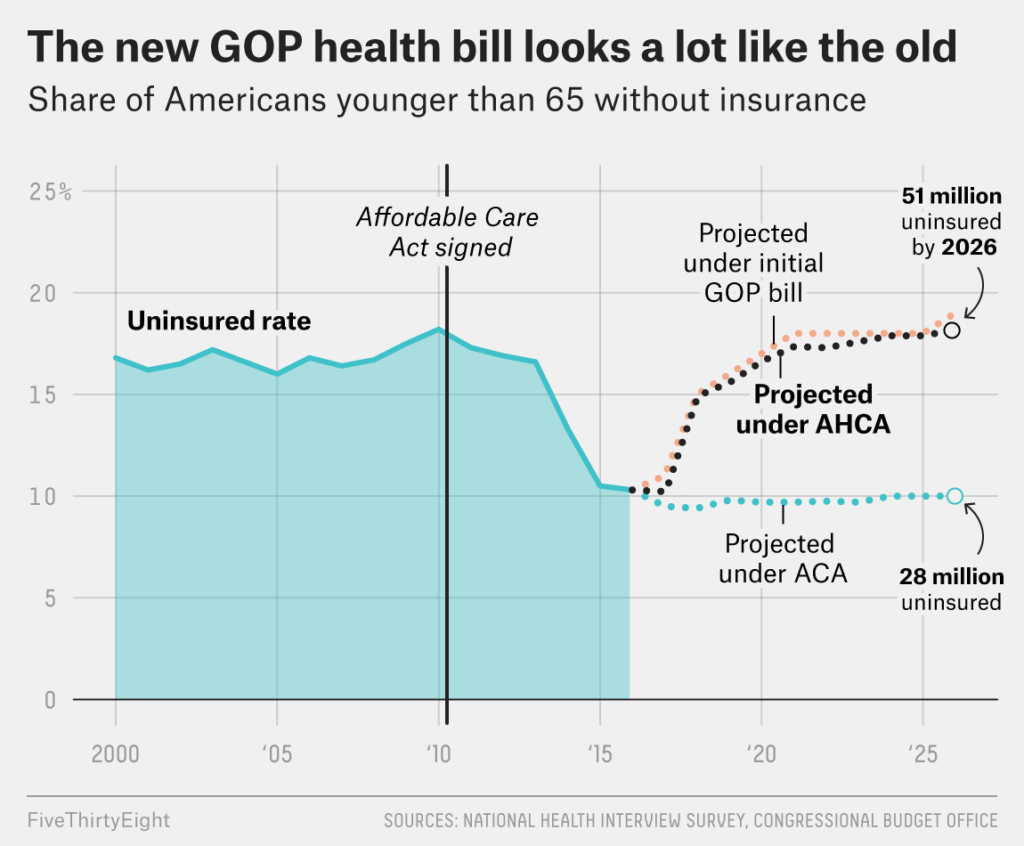
Millions of Americans could lose health insurance coverage if the proposed bill becomes law. The new legislation aims to restructure Medicaid and reduce federal funding for health programs, potentially affecting low-income individuals, families, and vulnerable populations. Experts warn that states may be forced to limit eligibility or reduce benefits due to tighter budgets.
Those relying on Medicaid expansion under the Affordable Care Act may face the greatest risk. Additionally, undocumented immigrants and people with preexisting conditions could see their access to care severely limited. As lawmakers debate the bill's future, uncertainty looms over millions who depend on government-supported health coverage for essential medical services.
Who Will Lose Health Insurance With the New Bill?
The potential impact of a new healthcare bill on insurance coverage has sparked widespread concern, particularly regarding which groups may lose their health insurance. While legislative details vary, proposed changes often target public health programs, employer mandates, or Medicaid expansion—areas that directly influence access to care for millions.
Low-income families, part-time workers, and individuals in states that adopted expanded Medicaid under the Affordable Care Act (ACA) are typically the most vulnerable to coverage loss if funding is reduced or eligibility criteria tightened. Additionally, people with pre-existing conditions could face higher premiums or limited options if protections are weakened.
The actual extent of insurance loss depends heavily on specific provisions in the bill, including subsidies, Medicaid block grants, and requirements for employer-sponsored insurance. Without robust replacement measures, any rollback of existing coverage could leave significant portions of the population uninsured.
Low-Income Individuals in Medicaid Expansion States
Populations in states that expanded Medicaid under the ACA are at high risk of losing health insurance if the new bill imposes per-capita caps or block grants on federal Medicaid funding.
These individuals, often earning just above the poverty line, rely on Medicaid for essential services like preventive care, mental health treatment, and hospitalization. If the new bill incentivizes states to restrict eligibility or reduce benefits to manage budget constraints, millions could be disenrolled.
Research from the Kaiser Family Foundation indicates that such changes could lead to up to 15 million people losing Medicaid coverage over a decade, particularly in Southern and Midwestern states where expansion is more recent or politically contested. The rollback would disproportionately affect children, pregnant women, and people with disabilities who are currently covered under expanded criteria.
| Group at Risk | Reason for Potential Loss | Potential Impact |
|---|---|---|
| Low-income adults (138% of poverty level) | Medicaid funding cuts or eligibility restrictions | Loss of preventive and chronic disease management services |
| Part-time and gig economy workers | Elimination of employer mandate or marketplace subsidies | Unaffordable private insurance premiums |
| People with pre-existing conditions | Reduced ACA protections or risk pool instability | Dramatic premium increases or coverage denial |
Individuals Relying on ACA Marketplace Subsidies
Millions of Americans who purchase insurance through the ACA marketplaces depend on federal subsidies to make premiums and deductibles affordable.
If the new bill reduces or eliminates these subsidies, middle- and lower-income enrollees could find themselves priced out of coverage. The subsidies are currently structured to cap insurance costs at a percentage of income, but a shift to flat tax credits or lump-sum grants could leave many unable to afford plans—especially in high-cost regions.
Furthermore, destabilizing the individual market by repealing the individual mandate without a viable alternative may lead insurers to exit the marketplace, resulting in fewer plan options and rising premiums. Urban and rural enrollees alike could see their access erode, with younger, healthier individuals opting out and older, sicker populations facing unaffordable rates.
Children and Families in Public Health Programs
Proposed changes to CHIP (Children’s Health Insurance Program) or Medicaid could threaten the coverage of over 9 million children who currently rely on these programs for pediatric care, immunizations, and developmental screenings. If funding is capped or reallocated under the new bill, states may be forced to reduce enrollment or limit benefits, leading to delayed care and worsening health outcomes.
Families with incomes too high for Medicaid but too low to afford private insurance are particularly vulnerable; a gap in coverage could result in increased emergency room use and untreated chronic conditions like asthma or diabetes. Schools and public health systems may also feel the strain as more children enter classrooms without up-to-date medical evaluations or mental health support.
Frequently Asked Questions
Who will lose health insurance under the new bill?
Individuals who receive subsidies for health insurance through the Affordable Care Act may lose coverage if the new bill reduces or eliminates those subsidies. People enrolled in Medicaid expansion programs in certain states could also be affected if funding is cut. Additionally, those with employer-sponsored insurance might lose benefits if companies adjust plans due to new regulations or cost shifts.
How will Medicaid recipients be impacted by the new legislation?
Medicaid recipients could lose coverage if the bill imposes work requirements, caps federal funding, or reduces enrollment eligibility. Some states may opt to scale back their Medicaid programs due to reduced federal support. Low-income adults, children, and disabled individuals relying on Medicaid may face disenrollment or reduced access to healthcare services depending on state-level implementation of the new rules.
Could people with pre-existing conditions lose insurance under the new bill?
If the new bill weakens protections for pre-existing conditions, some individuals might face higher premiums or be denied coverage by insurers. While current law guarantees coverage regardless of health status, changes to risk pools or state waivers could allow insurers to charge more or offer limited plans. This could effectively make insurance unaffordable, leading some to drop coverage despite having medical needs.
Will the elimination of the individual mandate affect insurance loss?
Yes, removing or weakening the individual mandate could lead to fewer healthy people enrolling in health insurance, destabilizing insurance markets. This might cause premiums to rise, prompting some insurers to exit the market. As a result, individuals—especially those in high-risk pools or rural areas—could lose access to affordable plans or face coverage gaps due to reduced market competition.

Leave a Reply