Usa Health Insurance System

The United States health insurance system is a complex network of public and private entities designed to help individuals manage the high costs of medical care.
Unlike many other developed nations, the U.S. does not have a universal healthcare system, relying instead on a mix of employer-sponsored plans, government programs like Medicare and Medicaid, and individual market policies. Navigating this system can be challenging, with varying coverage options, premiums, deductibles, and provider networks.
Understanding how health insurance works is essential for accessing timely and affordable care. This article explores the structure, key components, and challenges of the U.S. health insurance system, offering insight into how Americans obtain and use coverage.
 Auto Insurance Westfield
Auto Insurance WestfieldUnderstanding the U.S. Health Insurance System
The United States health insurance system is a complex network of public and private insurance providers that collectively aim to cover the medical expenses of individuals and families across the country.
Unlike many other developed nations, the U.S. does not have a universal healthcare system; instead, it relies on a mix of employer-sponsored insurance, government programs like Medicare and Medicaid, and individual market plans. Employer-based insurance is the most common form, with millions of Americans receiving coverage through their jobs.
Additionally, the Affordable Care Act (ACA), passed in 2010, significantly reshaped the landscape by creating health insurance marketplaces, expanding Medicaid eligibility in participating states, and implementing consumer protections such as banning denials due to pre-existing conditions. Despite these advancements, affordability, access, and coverage disparities remain persistent challenges, particularly for low-income populations and those residing in states that did not expand Medicaid.
Types of Health Insurance Plans in the U.S.
The U.S. health insurance market offers a variety of plans to meet different needs, each with distinct features, costs, and provider networks.
 Auto Manufacturer Insurance
Auto Manufacturer InsuranceThe most common types include Health Maintenance Organizations (HMOs), which require members to use a specific network of doctors and typically need referrals to see specialists; Preferred Provider Organizations (PPOs), which offer more flexibility to visit out-of-network providers at a higher cost; Exclusive Provider Organizations (EPOs), which balance cost and access by covering only in-network services except in emergencies; and High-Deductible Health Plans (HDHPs), which are often paired with Health Savings Accounts (HSAs) to help individuals save for medical expenses.
Coverage options also vary based on plan tiers such as bronze, silver, gold, and platinum, which indicate the percentage of costs covered by the insurer versus the enrollee. Understanding these differences is crucial for selecting a plan that aligns with one’s healthcare needs and financial capabilities.
| Plan Type | Network Flexibility | Cost Level | Specialist Access |
|---|---|---|---|
| HMO | Low (in-network only) | Lower premiums | Requires referral |
| PPO | High (in & out-of-network) | Higher premiums | No referral needed |
| EPO | Moderate (mostly in-network) | Moderate cost | Varies |
| HDHP with HSA | Varies by network | Low premiums, high deductible | Unrestricted |
Key Government Health Programs: Medicare and Medicaid
Two of the most important public health insurance programs in the U.S. are Medicare and Medicaid, both established in 1965 under the Social Security Act.
Medicare primarily serves Americans aged 65 and older, as well as certain younger individuals with disabilities or specific conditions like End-Stage Renal Disease (ESRD). It consists of several parts: Part A (hospital insurance), Part B (medical insurance), Part C (Medicare Advantage plans), and Part D (prescription drug coverage).
 Auto Owners Insurance Phone Number Claims
Auto Owners Insurance Phone Number ClaimsIn contrast, Medicaid is a needs-based program that provides coverage to low-income individuals and families, with eligibility and benefits varying by state. Some states have expanded Medicaid under the Affordable Care Act, significantly increasing access, while others have not, leading to coverage gaps. Both programs are jointly funded by federal and state governments but differ in administration and target populations.
Established by the Affordable Care Act, the Health Insurance Marketplace (also known as the Exchange) is a platform where individuals, families, and small businesses can compare and purchase health insurance plans.
Available at HealthCare.gov (or state-specific exchanges in some areas), the marketplace offers plans categorized by metal tiers—bronze, silver, gold, and platinum—each reflecting different levels of cost-sharing between the insurer and the enrollee. One of the key benefits of using the marketplace is access to premium tax credits and cost-sharing reductions for eligible individuals based on income, which can significantly reduce monthly premiums and out-of-pocket expenses.
Enrollment is typically limited to an annual Open Enrollment Period, although Special Enrollment Periods may be available for qualifying life events such as marriage, birth of a child, or loss of other coverage. Understanding how to use the marketplace effectively is essential for securing affordable and comprehensive health coverage.
How to Use the Health Insurance System: A Step-by-Step Guide
What type of health insurance system does the United States use?
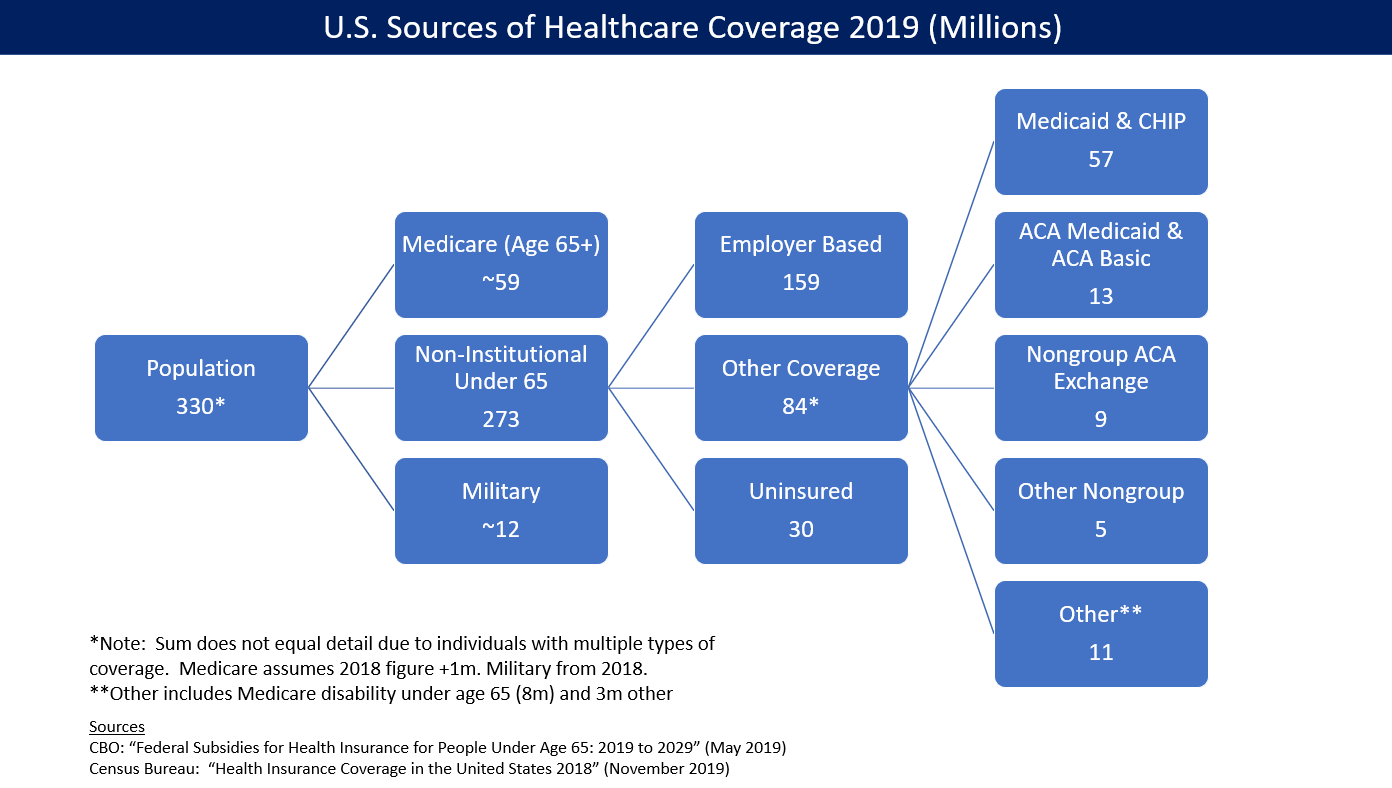
The United States operates a predominantly private, employer-based health insurance system, although it includes significant public programs for specific populations.
Unlike many developed countries that have universal healthcare systems funded by the government, the U.S. relies on a complex mix of private insurance plans, government-sponsored programs, and individual market arrangements. Most Americans receive health coverage through their employers, who negotiate plans with private insurers.
Additionally, federal and state programs such as Medicare, Medicaid, and the Children's Health Insurance Program (CHIP) provide coverage for seniors, low-income individuals, and children. The Affordable Care Act (ACA) expanded access by creating health insurance marketplaces and offering subsidies, but the system remains fragmented, with significant disparities in coverage and cost.
Key Components of the U.S. Health Insurance System
- The U.S. health insurance system is characterized by its reliance on private insurance, which covers approximately half of the population, often through employer-sponsored plans. These plans vary widely in terms of premiums, deductibles, and covered services, depending on the employer and insurer.
- Public programs such as Medicare provide health coverage to individuals aged 65 and older, as well as certain younger people with disabilities. Medicare is divided into parts: Part A covers hospital stays, Part B covers outpatient services, Part C (Medicare Advantage) offers private plan alternatives, and Part D provides prescription drug coverage.
- Medicaid, jointly funded by federal and state governments, offers coverage to low-income individuals and families. Eligibility and benefits can vary significantly between states, and the program was expanded in many states under the Affordable Care Act to include more low-income adults.
Role of the Affordable Care Act (ACA)
- Enacted in 2010, the Affordable Care Act aimed to increase access to health insurance, reduce uninsured rates, and improve healthcare quality. A central element was the creation of Health Insurance Marketplaces, where individuals and small businesses can compare and purchase plans, often with income-based subsidies.
- The ACA introduced important consumer protections, such as prohibiting insurers from denying coverage based on pre-existing conditions and allowing young adults to stay on their parents' plans until age 26. It also mandated that most Americans have health insurance or face a tax penalty, although this individual mandate penalty was reduced to zero at the federal level in 2019.
- As a result of the ACA, millions gained coverage, and the uninsured rate dropped significantly. However, challenges remain, including high premiums in some areas, limited provider networks, and political debates over the law's structure and sustainability.
Challenges and Inequities in the U.S. System
- Despite significant spending on healthcare, the U.S. faces persistent inequities in access and outcomes. Millions of Americans remain uninsured or underinsured, particularly in states that chose not to expand Medicaid, leaving a coverage gap for low-income adults who earn too much for traditional Medicaid but too little for marketplace subsidies.
- Healthcare costs in the U.S. are among the highest in the world, driven by high administrative expenses, drug prices, and provider fees. Patients often face surprise medical bills, especially when treated by out-of-network providers, even in emergency situations.
- The fragmented nature of the insurance system leads to inefficiencies and confusion for consumers. Individuals must navigate a complex array of plans, coverage rules, and billing practices, which can deter timely care and contribute to poor health outcomes compared to other high-income countries.
Is healthcare fully covered in the U.S. for those with health insurance?
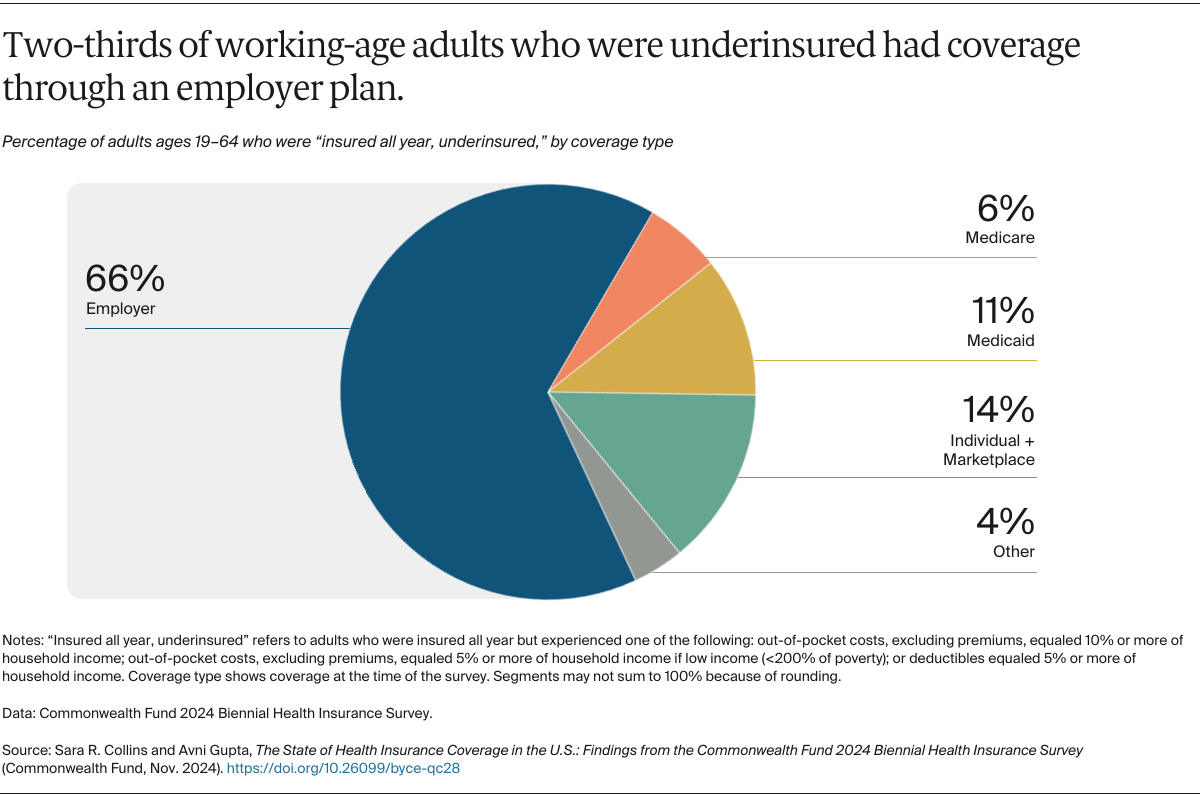
No, healthcare is not fully covered in the U.S. for those with health insurance. While having health insurance significantly reduces out-of-pocket costs, most insurance plans require patients to pay certain amounts such as premiums, deductibles, copayments, and coinsurance.
Additionally, not all medical services or treatments are included in every plan, and some may require prior authorization or be subject to coverage limits. The extent of coverage varies greatly depending on the type of insurance—such as employer-sponsored plans, Medicare, Medicaid, or marketplace plans under the Affordable Care Act—meaning individuals often still face substantial healthcare expenses even with insurance.
What Costs Are Typically Not Fully Covered by Health Insurance?
- Most health insurance plans in the U.S. require enrollees to pay monthly premiums, which are fixed payments made regardless of whether medical services are used during the month.
- Deductibles represent the amount a person must pay out of pocket before the insurance company begins to cover services, and these can range from a few hundred to several thousand dollars annually.
- Even after meeting the deductible, patients usually pay copayments (fixed fees for services like doctor visits) or coinsurance (a percentage of the service cost), meaning the insurance does not cover 100% of the charges.
How Do Insurance Plan Types Affect Coverage Gaps?
- Employer-sponsored insurance often provides comprehensive benefits, but the specifics—like network restrictions, formulary drugs, and specialist referrals—can limit what is fully covered.
- Plans purchased through the Health Insurance Marketplace vary by metal tier (bronze, silver, gold, platinum), with lower-tier plans covering a smaller percentage of costs and leaving more financial responsibility to the individual.
- Medicare covers many services for seniors and some disabled individuals, but it does not include long-term care, most dental care, vision exams, hearing aids, or routine foot care, leading beneficiaries to seek supplemental policies.
What Services Are Commonly Excluded or Partially Covered?
- Mental health and substance use disorder services, while required to be covered under the Affordable Care Act, may have limitations such as a restricted number of therapy sessions or higher copays.
- Prescription drugs are covered under most plans, but the level of coverage depends on the drug’s placement in the plan’s formulary, with some medications requiring prior authorization or step therapy.
- Alternative treatments like acupuncture, chiropractic care, or weight-loss surgeries may only be partially covered or excluded altogether, especially if deemed not medically necessary by the insurer.
What is the average cost of comprehensive health insurance in the U.S.?

The average cost of comprehensive health insurance in the U.S. varies significantly depending on multiple factors such as geographic location, age, income level, employer contributions, and the type of plan selected.
As of 2023, the average monthly premium for individual coverage under an employer-sponsored plan was approximately $501, while family plans averaged about $1,392 per month. These figures represent contributions from both employers and employees, with employers typically covering about 73% of the premium for single coverage and 67% for family plans.
For those purchasing plans through the Health Insurance Marketplace established under the Affordable Care Act (ACA), premiums can differ widely, but subsidies are often available to lower-income individuals and families, reducing the effective cost. Additionally, comprehensive plans with lower deductibles and broader provider networks tend to have higher premiums compared to high-deductible health plans.
Factors Influencing the Cost of Comprehensive Health Insurance
- Geographic location plays a crucial role in determining insurance costs, as premiums can be substantially higher in urban areas or states with elevated healthcare delivery costs. For example, residents in states like New York or California often pay more than those in rural states such as Idaho or Arkansas due to variations in provider rates, cost of living, and state regulations.
- Age is another significant factor; insurers are allowed to charge older adults up to three times more than younger individuals for the same plan. A 60-year-old may pay significantly more than a 25-year-old for identical coverage, reflecting higher expected healthcare utilization among older populations.
- Income level affects out-of-pocket expenses primarily through subsidy eligibility on the ACA Marketplace. Individuals and families earning between 100% and 400% of the federal poverty level may qualify for premium tax credits, which can drastically reduce monthly payments and make comprehensive coverage more affordable.
Differences Between Employer-Sponsored and Marketplace Plans
- Employer-sponsored health insurance remains the most common form of coverage in the U.S., and these plans generally offer lower premiums for employees due to shared costs with the employer. The group purchasing power of large companies allows for negotiated rates with insurers and healthcare providers, leading to more favorable pricing compared to individual market plans.
- Plans available on the ACA Marketplace cater to individuals who do not have access to job-based coverage. While these plans offer essential health benefits and come in various metal tiers (bronze, silver, gold, platinum), premiums tend to be higher without employer contributions. However, cost-sharing reductions and tax credits can help mitigate expenses for qualifying enrollees.
- Employer plans often feature richer benefits and lower deductibles than comparable individual plans. Comprehensive employer plans may include broader networks, lower co-pays, and additional wellness programs, which justify their higher perceived value despite the growing cost burden on both employers and workers.
What Is Included in a Comprehensive Health Insurance Plan?
- Comprehensive health insurance typically covers ten essential health benefits mandated by the Affordable Care Act, including emergency services, hospitalization, maternity care, mental health and substance use disorder treatment, prescription drugs, and preventive services. These benefits ensure that policyholders have access to a wide range of medical needs without facing excessive out-of-pocket charges.
- Preventive care is fully covered at no additional cost to the insured, even if the deductible has not been met. This includes annual check-ups, vaccinations, cancer screenings, and wellness visits, promoting early detection and long-term health management.
- Comprehensive plans usually have lower deductibles, co-insurance, and out-of-pocket maximums compared to high-deductible plans. This structure reduces financial risk during medical emergencies or chronic illness management, making them particularly valuable for individuals with ongoing healthcare needs or families seeking robust protection.
Frequently Asked Questions
What is the U.S. health insurance system?
The U.S. health insurance system is a mix of private and public insurance programs. Most people get coverage through employers, while others buy plans on the marketplace or qualify for government programs like Medicare or Medicaid. There's no universal healthcare, so individuals must enroll in a plan to access affordable medical services. Coverage varies by plan, and costs include premiums, deductibles, and copays.
How do I enroll in a health insurance plan?
You can enroll during the annual Open Enrollment Period or after qualifying life events like job loss or marriage. Employer-sponsored plans typically enroll during work benefits orientation. For marketplace plans, visit HealthCare.gov to compare and sign up. You'll need personal details, income information, and household size. Special enrollment periods may apply depending on your situation, so apply promptly to avoid coverage gaps.
What is the difference between Medicare and Medicaid?
Medicare is a federal program primarily for people aged 65 and older, regardless of income. It includes hospital (Part A) and medical (Part B) coverage, with optional Part D for prescriptions. Medicaid is a joint federal and state program for low-income individuals and families. Eligibility and benefits vary by state. Some people qualify for both, known as dual eligibles, receiving comprehensive coverage.
Can I keep my doctor with my insurance plan?
It depends on your plan's network. HMO and POS plans usually require you to use in-network providers, except in emergencies. PPO plans offer more flexibility to see out-of-network doctors at a higher cost. Check your insurer’s provider directory or ask your doctor if they accept your insurance. Staying in-network typically lowers your costs, so verify before scheduling appointments to avoid unexpected bills.

Leave a Reply